Examination and Treatment of Achilles Tendon: 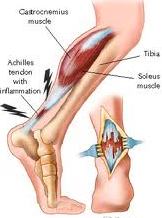
Acute tendon rupture is most common among men aged 30-50 years (mean age, 40 years) it causes sudden severe disability.
Achilles tendon injuries tendinopathy may arise with increased training volume or intensity but may also arise insidiously. Because the prognosis for midportion Achilles tendinopathy is much better than for insertional tendinopathy, these conditions should be distinguished clinically. The condition that was previously called ‘Achilles tendinitis‘ is not truly an inflammatory condition and, thus, should be referred to as ‘Achilles tendinopathy’. The main differential diagnoses of gradual onset pain in the Achilles region arise from the neighboring anatomy.
There are two bursae in this region:
- The Retrocalcaneal Bursa
- The Achilles Bursa
1. The Retrocalcaneal Bursa: Retrocalcaneal Bursa lies between the posterior aspect of the calcaneus and the insertion of the Achilles tendon.
2. The Achilles Bursa: Achilles Bursa lies between the insersion of the Achilles tendon and the skin.
The posterior process of the talus or a discrete anatomical variant, the os trigonum, can each be involved in posterior impingement syndrome. This is most commonly seen in ballet dancers but occurs occasionally in sprinters and in football players. Other, much less common differential diagnoses include dislocation of the peroneal tendons, an accessory soleus muscle, irritation, or neuroma of the sural nerve, and systemic inflammatory disease. These pathologies cause pain in and also around the Achilles tendon; true tendon pain is almost always confined to the tendon itself. In adolescents, it is important to consider the diagnosis of Sever’s lesion, a traction apophysitis at the insertion of the Achilles tendon into the calcaneus. Referred pain is a very rare cause of pain in the Achilles region.
History
- The athlete with overuse tendinopathy notices a gradual development of symptoms and typically complains of pain and morning stiffness after increasing activity level.
- Pain diminishes with walking about or applying heat. In most cases, pain diminishes during training, only to recur several hours afterwards.
- The onset of pain is usually more sudden in a partial tear of the Achilles tendon. In this uncommon condition, pain may be more disabling in the short term.
- As the histological abnormality in a partial tear and in overuse tendinopathy are identical, we do not emphasize the distinction other than to suggest that time to recovery may be longer in cases of partial tear.
Examination
Palpate the painful area for tenderness, thickening, and crepitus. If the Achilles tendon seems to be the cause of pain, and the examiner is confident that the tendon is intact, the examination should aim to provoke tendon pain during tendon loading activity. These functional tests provide a baseline against which treatment response can be compared. Another method of monitoring the clinical progress of Achilles tendinopathy is to use the VISA questionnaire. This is simple questionnaire takes less than 5 minutes to complete and once patients are familiar with it they can complete most of it themselves.
Examination involves:
1. Observation
- Standing
- Walking
- Prone
2. Active movements
- Plantarflexion
- Dorsiflexion
3. Passive movements
- Plantarflexion
- Plantarflexion with overpressure
- Dorsiflexion
- Subtalar joint
- Muscle stretch
- Gastrocnemius
- Soleus
4. Resisted movements
- Plantarflexion- calf raises
5. Functional tests
- Single- leg calf raises
- Hop
- Eccentric drop
6. Palpation
- Achilles tendon
- Retrocalcaneal bursa
- Posterior talus
- Calf muscle
7. Special test
- Prone inspection for tendon rupture
- Simmond’s Calf squeeze test
- Biomechanical assessment
Investigations and Treatment of Achilles Tendons
- Plain radiographs are of limited value but, if symptoms are longstanding, they may reveal a Haglund’s deformity, a prominent superior projection of the calcaneus, or spurs projecting into the tendon.
- Posterior impingement can be shown radiographically using functional views. X-ray may reveal calcification in the tendon itself but, unless severe, this can be asymptomatic.
- In symptomatic patients, both ultrasound and MRI often reveal an abnormal signal in the Achilles tendon that generally corresponds with the histopathology of tendinosis.
- Ultrasound and MRI can help distinguish different causes of pain in the Achilles region.
- Achilles tendon insertion is abnormal in patients with pain at the distal tendon.
- It may also provide a target for treatment. Because of the variability in imaging and its inconsistent clinical correlation, the results of imaging should not dominate clinical decision making variation in symptoms such as morning stiffness and load pain should direct treatment modification. Studies in many tendons have indicated that clinical outcomes are independent of imaging and change in imaging.
Achilles tendinitis is a typical situation that causes discomfort along the returning of the leg near the returning heel. Active Physical Therapy is the best Physical Therapy Center which is specialists in treating Ankle Sprains, Knee and Ankle Injuries, Bursitis/Tendonitis etc. Call now at: 301-662-9335